I spent 30 days peering inside my blood 24/7, thanks to a continuous glucose monitor (CGM). This experience completely changed my perspective on my metabolic health, how food impacts my body, and how small lifestyle changes can have a large impact on my glucose levels and in turn my health.
If you're CGM-curious, this article is for you. We'll explore the benefits of CGMs, why glucose levels are crucial for longevity, what glucose levels are best for health, and most importantly, the key lessons I learned from my month-long experiment that can help you optimize your health with or without using a CGM yourself.
First let's dive into the background on CGMs and why we should care about our blood glucose but if you are just looking for the key takeaways and what you can do to improve your metabolic health skip to HERE.
📑 Table of Contents 📑
1. What is a CGM?
2. Why Use a CGM
3. What I hoped to learn from my CGM experiment
4. Research Review -What Glucose Levels are Optimal?
5. Target Glucose/CGM Values For Longevity
6. Glucose Metrics With Longevity Targets
7. My CGM Experiment Results
8. Key Take-Aways From My CGM Experiment
9. What you should know before using a CGM
10. Summary
What is a CGM?
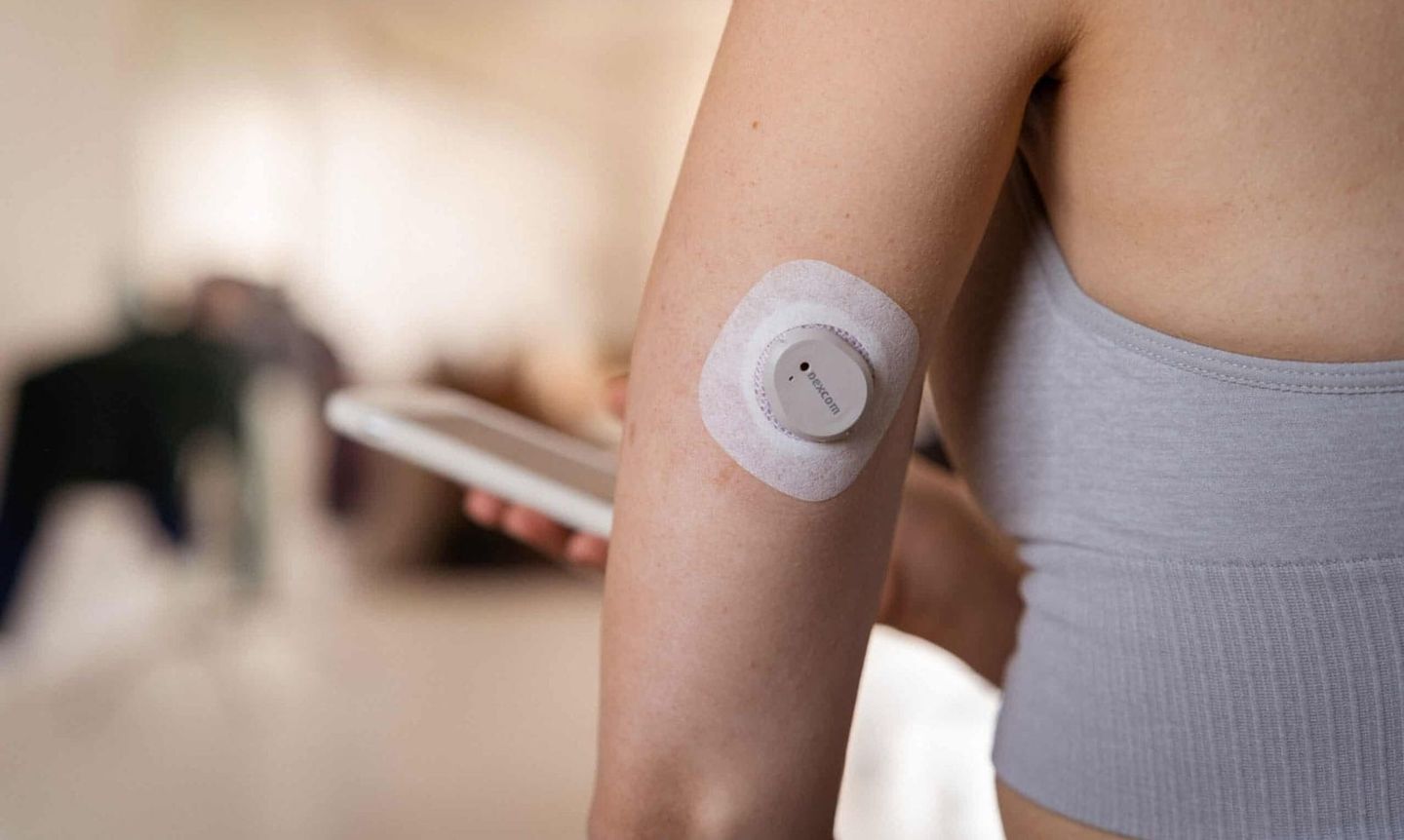
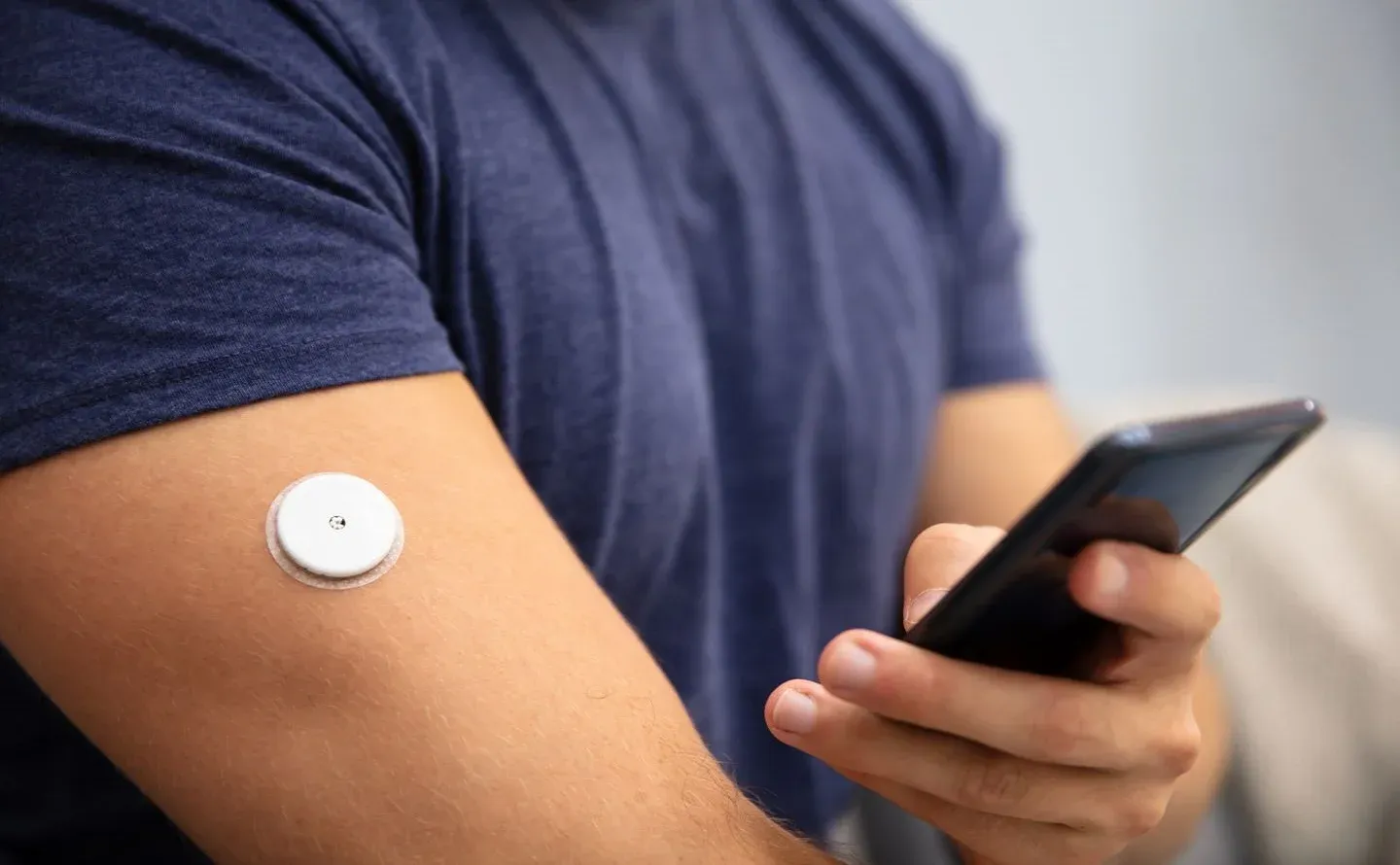
For those unfamiliar, a continuous glucose monitor (CGM) is a small device worn on the back of your arm. A tiny sensor, inserted just under the skin, measures your blood glucose levels continuously throughout the day and sends this data to your phone. Each sensor lasts for ten days; therefore, I used three sensors during my 30-day experiment.
Applying the CGM is a simple process done at home and takes less than ten minutes.
Why Use a CGM?
Understanding your body's glucose levels and how it changes is our best tool for understanding and improving metabolic health.
Metabolic health, at its core, is how effectively your body converts nutrients into energy. When we consume carbohydrates, glucose levels rise, prompting the body to release insulin. Insulin's role is to lower glucose levels, as prolonged high glucose is toxic and damages the body in various ways, including contributing to inflammation and oxidative stress. This system is always trying to maintain homeostasis and when over taxed by chronically high insulin the body becomes insulin resistant which results in what we call type 2 diabetes. Diabetes and its precursor pre-diabetes is diagnosed by abnormalities in glucose and insulin levels. Specifically, the duration and height of glucose spikes after a given amount of carbohydrates indicates how efficiently ones body manages glucose, produces insulin, and at a cellular level how your beta cells are functioning.
The information provided by a CGM is particularly relevant given the growing prevalence of metabolic disorders. One-third of Americans have prediabetes, and the rate of type 2 diabetes is rapidly increasing [source]. These statistics underscore the importance of understanding and managing glucose levels to reduce the risk of developing metabolic dysfunction, which greatly increases one's risk of the most deadly chronic diseases – including cancer, heart disease, and neurodegenerative diseases like Alzheimer's. To emphasize this point, type 2 diabetes is associated with a 40% increase in all-cause mortality [source]. For those seeking to maximize healthspan and lifespan, maintaining optimal metabolic health should be a primary goal.
A CGM is the best tool for understanding one's state of metabolic health as it shows glucose levels over time and allows one to identify any issues with this system before irreversible damage is done. The glucose response curve from my CGM, as shown below, provides a visual representation of how my body is reacting to meals and other things like exercise and sleep
By leveraging the insights provided by a CGM, individuals can take proactive steps to optimize their metabolic health, reduce their risk of metabolic conditions and chronic disease, and enhance their potential healthspan and lifespan. (Check out my Peter Attia Outlive Summary for more information on these terms)
What I hoped to learn from my CGM experiment
I hoped that the data from my month of using a CGM would allow me to better understand the state of metabolic health, see how different foods impact my glucose levels, and find practical ways that I could improve my metabolic health.
The key thing that pushed me to actually pony up the money for this CGM experiment was that my recent bloodwork showed my Hba1c (in simple terms is a measure of average glucose over the past 90 days) was 5.6 which is on the borderline pre diabetic levels. As a youngish person who considers themselves in top notch health, exercises religiously, eats generally pretty well, and has great blood markers, I wanted to figure out what was going on and if I should be concerned. I also wanted to see how my Hba1c would change with the key lessons I learned from using a CGM – the difference was larger than I expected.
To answer these questions I turned to my new friend the Dexcon G7. With this baby I’ll answer all these questions and clearly know what’s going on with me…...right?
Research Review - What Glucose Levels are Optimal?
If you want to skip to my results and main takeaways see them HERE
As I got my first glucose readings I realized I didn't know what to be looking for in terms of optimal levels. This drove me to dive into the research on glucose levels, their relationship with health, and why the idea that lower glucose is better seems to be in vogue among health influencers and people in the longevity space.
This literature review was more than I initially signed up for and it soon became an all consuming search for the truth in a sea of suspect sources. The main issue that I found was that a majority of research on how glucose impacts health has been done on people with diabetes and the research for healthy individuals is less robust. Additionally the data we do have is observational vs. a true blind experiments so please keep that in mind as we discuss these studies.
Research Highlights
- Over a lifetime, staying out of the diabetic range and keeping glucose in a healthy range and not becoming insulin resistant is one of the most important things you can do for health and longevity. As stated, having diabetes or metabolic dysfunction is a major risk factor for many diseases. Understanding where your current metabolic health stands can be done with: fasting glucose, fasting insulin, an OGTT, triglyceride to HDL ratio, and hba1c. However, a CGM is going to give you the most granularity here and provide direct feedback on how lifestyle and diet changes impact your glucose.
- Keeping postprandial glucose levels in a lower range may have positive health outcomes and in absence of perfect data sources would bias towards lower average glucose if trying to optimize your health and lifespan. Below is some evidence to back up this claim.
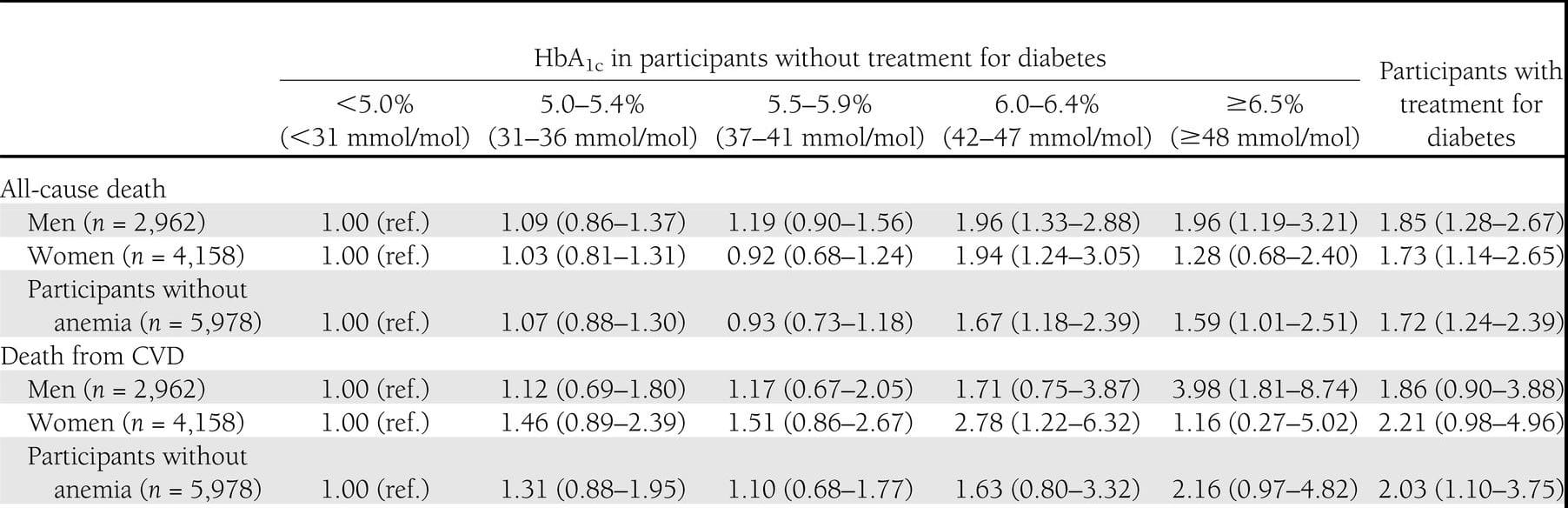
One larger study showed that looking at 200,000 people with an average age of 59 that risk of death increased with hba1c even within healthy ranges. Similarly this study from Japan showed the same general trend in increased mortality risk with higher average glucose as measured by hba1c. Similarly, this study showed that for men fasting glucose >85 lead to worse risk of cardiovascular disease.
Lastly this study shows that higher normal fasting glucose levels have been independently linked to increased arterial stiffness, which is a known correlative risk factor for cardiovascular events.
These studies are far from perfect but do show a trend of increased risk for various diseases as one's Hba1c increases. The effect of healthy vs. diabetic levels is very clear but this trend also seems to hold within non-diabetic ranges making a good argument that if longevity and maximizing health span is your goal that a lower hba1c and average glucose is better.
- Reducing the magnitude of postprandial spikes (how high your glucose peaks post meal) may lead to better health outcomes.
One key study in this area showed that less frequent and smaller magnitude glucose spikes resulted in reduced cardiovascular disease and inflammation markers. This study shows that changes in glucose were more likely to result in these negative impact than higher average glucose. I would be remiss not to call out that this study was looking at induced glucose spikes of long 6 hour durations which is far from the more transient 1-2 hour spikes seen in health individuals.
2 hours post meal glucose levels also seem to correlate to death risk per this study from Taiwan.
The last piece of data that makes me want to keep glucose levels low is the research on Acarbose [study1, study2] which is a diabetes drug that lowers glucose. These studies in mice show that individuals on them live longer than expected even when controlling for other factors that median survival of the males and females increased 22% and 5% respectively. These groups did not have difference Hba1cs which leads one to think if the drugs ability to buffer the glucose peak height may be causing this life extension. - Don’t over focus on blood glucose and ignore other aspects of health as this is one piece of the health puzzle and since it’s easier to measure in real-time, thanks to our CGM, it can easily distract from other critical things.
Target Glucose/CGM Values For Longevity
Alright with that more research section out of the way let’s get back to more pragmatic discussion on what all this CGM data means and glucose level targets for longevity and optimal health.
I know the first thing I did once saw my first CGM readings was ask what is the "best" glucose level, the max spike I should see after a meal, and what my goals should be with these values. The research on this is less robust than I would like and blood glucose is much more complex than “X is an ideal number”. However, let's try and answer this with information in hand.
Glucose Metrics With Longevity Targets
Here are the key metrics you would have access to with a CGM and a few other blood tests that measure metabolic health. I have included the targets for these metrics that I am aiming for in the interest of maximizing my healthspan based on the research in previous section. These values are the best I could find for health optimization, based on limited research, but I suspect there is more variability than shown below depending on many personal factors. These targets are biased towards the lower end as don't see any harm being on being closer to lower range for blood glucose. Lastly, don't overdo it on these targets and I wasn't able to have optimal ranges all the time. If you are not insulin resistant don't let glucose levels get in the way of enjoying your life too much.
Average Glucose - CGMs output average glucose values throughout the day and this is a key metric that ties to all the research on hba1c and average lower glucose appearing to reduce the risk of many diseases. Prediabetes is defined by a hba1c of 5.7 so an average glucose below 114mg/dl is needed to be in what is clinically defined as healthy range but if trying to be optimal here would aim for an hba1c less than or equal to 5.0 and average glucose of 97mg/dl or less.
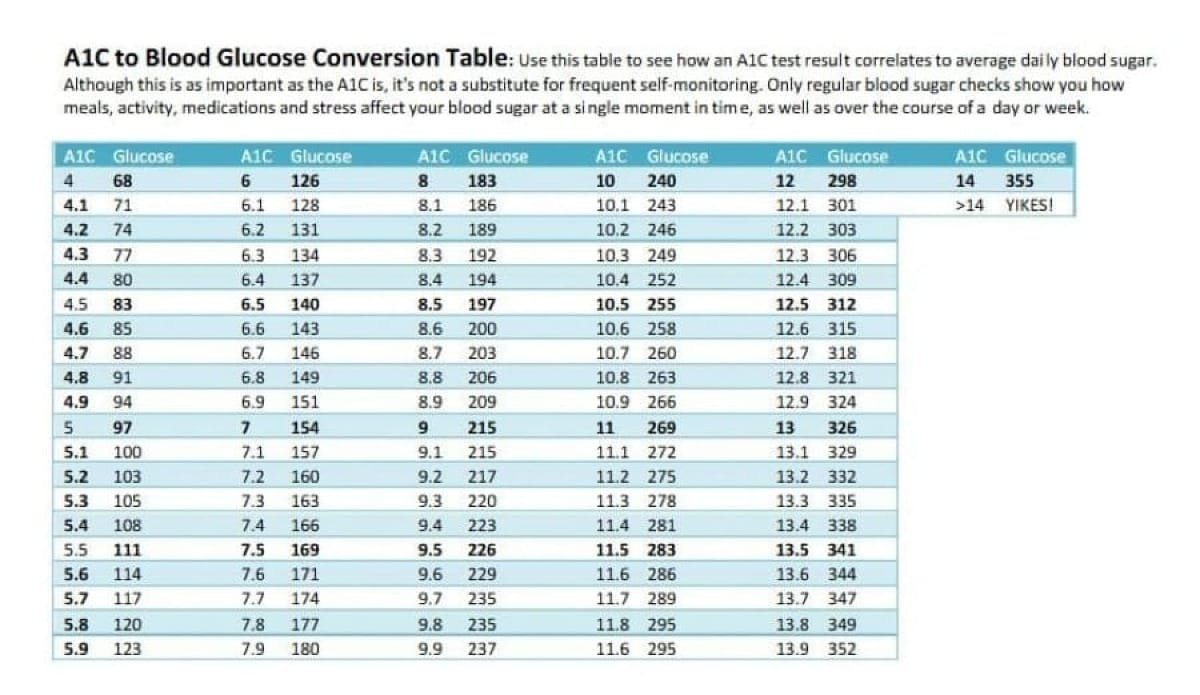
Postpandrial Glucose Spike - This is how high one's glucose gets after eating a meal. This generally happens 1-1.5 hours post meal and for optimal health would try to limit these peaks to under 140mg/dl for a vast majority of meals and aim for under 130mg/dl for most meals.
I want to be clear that glucose spiking up or beyond 140mg/dl is perfectly fine and as long as it comes back down quickly and does not stay elevated your insulin system is working as designed. This should not scare you but also may not be optimal for long term health based on the studies we have looked at. These are nice targets to have in mind but I know I had a couple of meals that spiked me above 140mg/dl during my experiment which is not a big deal.
Lastly the length of elevated glucose levels matters more than spike and based on expert options and my research personally target my post meal glucose, assuming I’m starting around 90mg/dl, is <140 mg/dl at 30 min, <130mg/dl at 60min, and <120mg/dl at 90 min
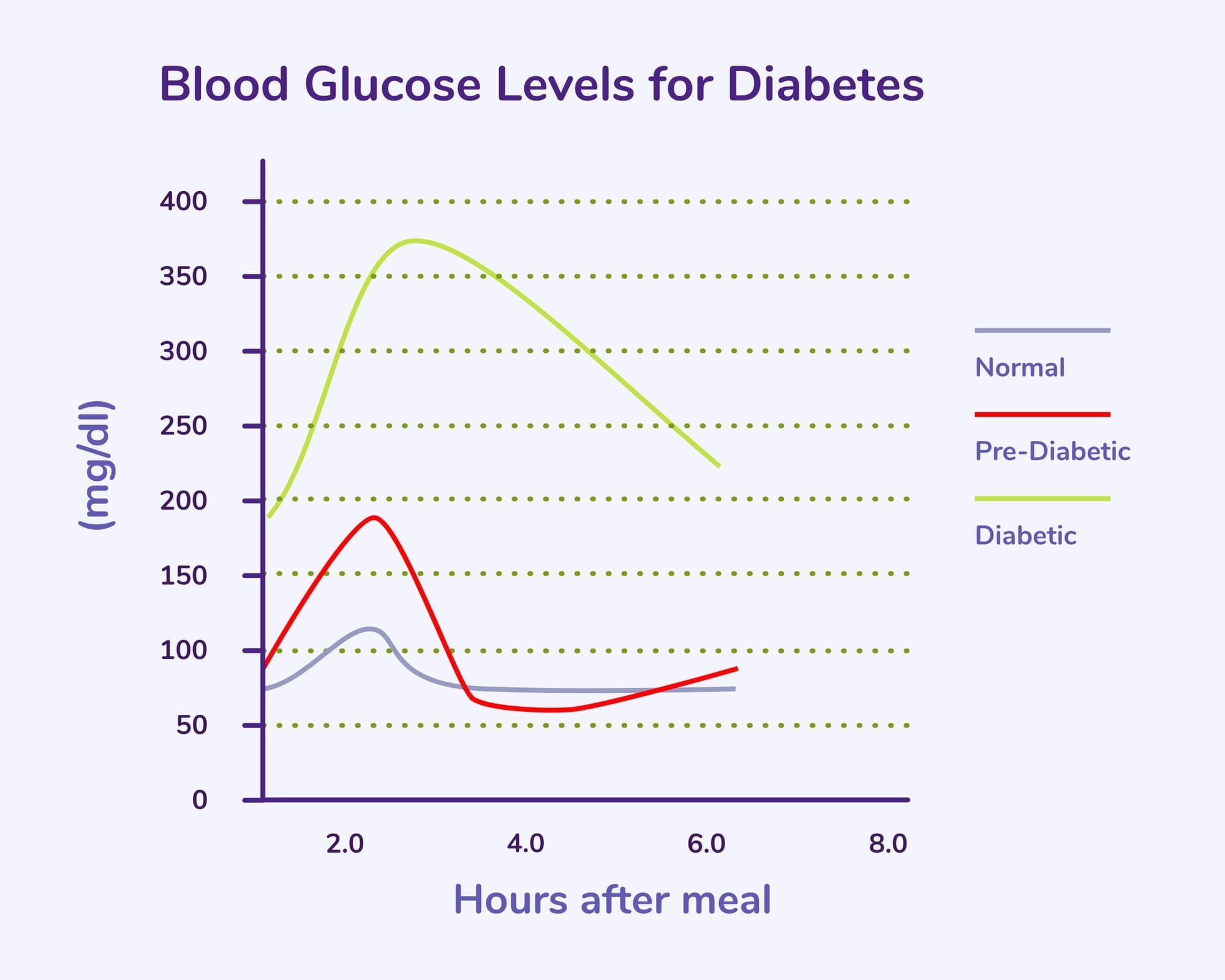
TIR- Time in range which is the time your glucose is in target range. For optimal I would say you want to keep glucose 70-100 mg/dl for ~85% of time.
Glucose variability- Large swings or changes in glucose can cause issues so smoother glucose responses are preferred. A CGM should output the variability or standard deviation which I aim to keep under 10mg/dl
Fasting glucose- fasting glucose below 90mg/dl is ideal but be aware sleep quality and stress can impact this so measuring this only one time can sometimes be misleading. Many people have what is called the “dawn phenomenon” where their glucose rises in the morning without food so if your levels look high wait a couple hours without food and check again for more accurate fasting level.
Hba1c - This is a blood test that tries to measure ones average glucose over 3 months and is an easy metric to track. I will say I saw a large disconnect between my hba1c estimated average glucose and levels measured by CGM or predicted by fasting glucose and insulin. I think this is a great metric to understand changes to glucose but not reliable for many people as single metric.
Other Tests - For understanding metabolic health beyond this work with a doctor but other tests that can provide insight are the OGTT, LP-IR, Beta cell function, and even LDL/Triglyceride ratio.
My CGM Experiment Results
Below are my metrics from this month long CGM experiment
- Average glucose= 91
- Standard Deviation = 12 mg/dl
- TIR = 96% between 70-120 mg/dl
- Max glucose = 155 mg/dl
- Hba1c before CGM experiment = 5.6%
- My average glucose would be an HBa1c of 4.8% hence why hba1c can be misleading for some individuals
- Hba1c after CGM experiment = 5.2% (3 months later)
- Fasting glucose before CGM experiment = 88
- Fasting Glucose after CGM experiment = 82 (3 months later)
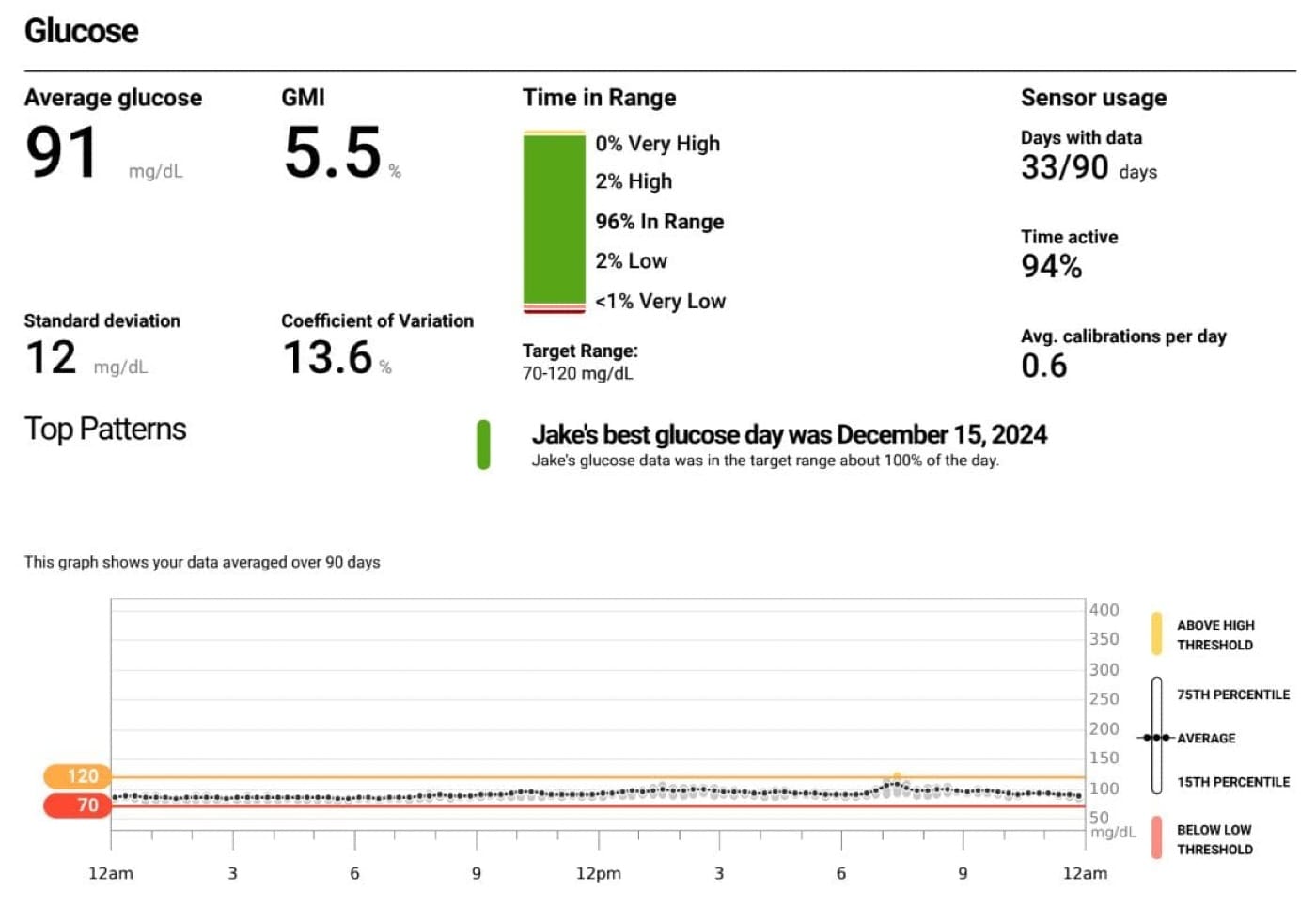
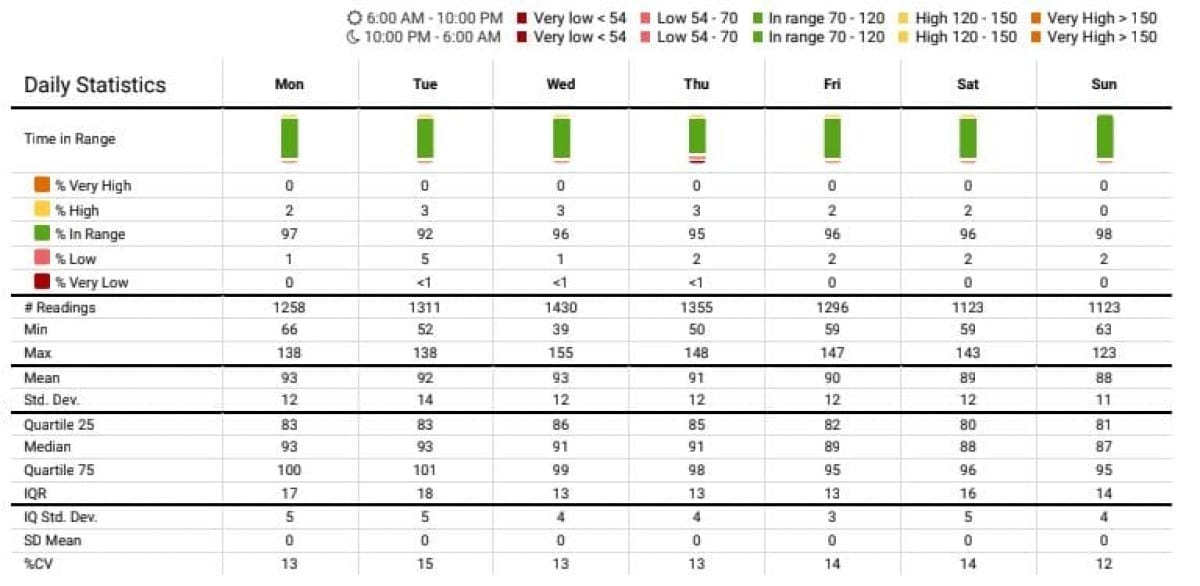
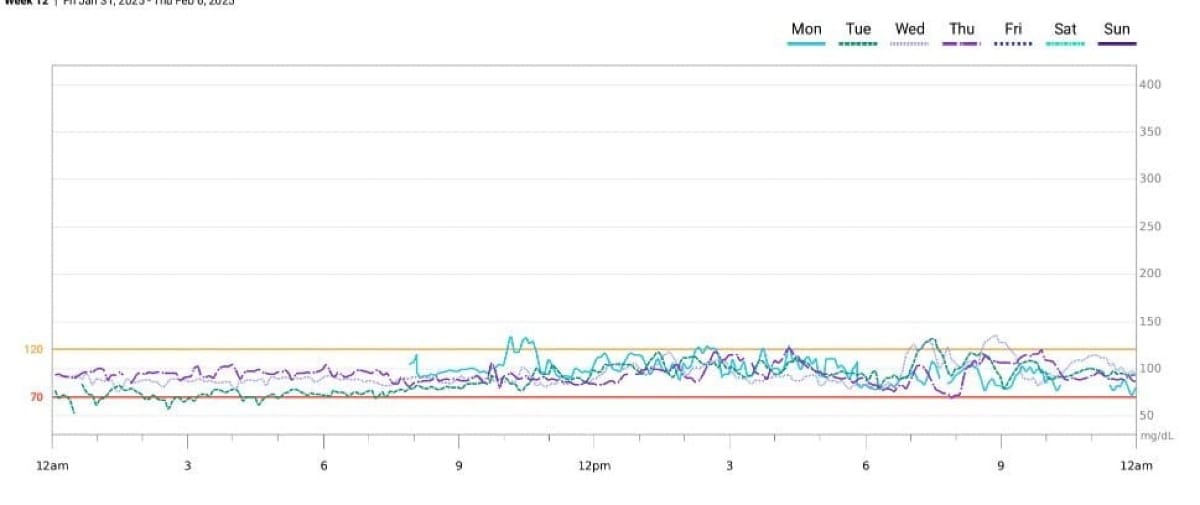
Overall I feel pretty metabolically healthy after my experiment but had more spikes above 140mg/dl than I would prefer and think I have room for improvement. After implementing some changes to my diet and lifestyle I did see a reduction in my hba1c and fasting glucose in my next blood test which was 3 months later (5.6 to 5.2) – The lessons I learned appear to be working.
Key Take-Aways From My CGM Experiment
After reading for what I’m sure feels like hours let’s finally get to the key takeaways from this experiment and the things you can do to improve your metabolic health, even without getting a CGM .
- Taking a walk, even a short one, after eating. A walk or any movement post meal has a big impact on the magnitude of your glucose spike and glucose control throughout the day. The research I found showed a postprandial glucose reduction of 10%-30% and reduction in average glucose as well. Anecdotally my largest glucose spikes were always after large carb heavy dinners and sitting on the couch with no movement.
- Focus on building more muscle mass for improved glucose control. Lean muscle is a major glucose sink, actively taking up glucose from the blood for energy and storage as glycogen. This increased capacity helps buffer postprandial glucose spikes, and is one of the lesser talked about benefits of resistance training for both men and women.
- Meal timing can have an impact on glucose levels. For example, moving more carbs earlier in the day around physical activity allowed me to reduce average glucose throughout the day as the activity reduced my glucose spikes and the more even spread of calories throughout the day helped me avoid a massive evening meal where I saw my highest glucose levels.
- Food matters. Refined carbohydrates result in much larger glucose spikes than less refined carbs with more fiber. I saw a large difference in the magnitude of my postprandial glucose levels when switching from white rice to brown rice for example.
The macronutrient makeup and order you eat your food also has a big impact on glucose response. Try to avoid meals of pure carbohydrates as eating meals with fiber, protein and fat greatly reduces one's glucose spike. If you really want to optimize this, eat protein, fats, and fiber before your carbohydrates as this meal timing reduces mean glucose spike for similar meals. For example, I found eating a salad before dinner and then starting my meal with the protein the best order for reducing my glucose levels. - Sleep and Stress impact glucose more than you think. I noticed that after just one night of poor quality or short duration sleep my average glucose much higher the next day and the days and weeks I had many stressors also showed up as higher average glucose and much less smooth glucose response curves to meals.
- Look at time restricted eating to reduce average glucose. Your glucose takes a while to return to baseline so skipping meals and allowing your body time to return to baseline glucose levels can help optimize your average glucose and metrics we discussed. You can also achieve this by limiting carbohydrates from certain meals vs. strictly not eating. You can imagine someone who is snacking on foods high in carbohydrates every couple of hours will have a higher average glucose as their body never fully gets back to baseline levels outside of sleep.
- Hba1c can be very misleading and in my case did a poor job of predicting my average glucose. This seems common among athletes and people that genetically hold onto red blood cells longer.
- Vigorous exercise can increase glucose levels. This can be especially true of fasted exercise for some people.
- In terms of supplements Berberine, ideally taken 30 min before a meal, can buffer glucose response. Alpha-Lipoic Acid (ALA) also has been shown to help improve insulin sensitivity.
- Higher glucose levels, if not insulin resistant, are not the end of the world and I did not find any research clearly showing my average glucose of 96, fasting around 88, and occasional spikes above 140 being cause for concern.
Your body elevating your glucose is perfectly normal and if wearing a CGM it’s easy to develop an unhealthy reaction to seeing an elevated glucose level. The glucose response curve and time to return to baseline is much more critical that spike magnitude when trying to understand metabolic health and insulin resistance.
What you should know before using a CGM
- Calibrate your CGM with a finger prick glucose device (I use this one) as the CGM drifts out of accuracy in my experience and also needs multiple calibrations in the first few days to be accurate. I have seen many people online think they are dying as CGM is showing glucose levels 20-30 points higher than reality due to the lack of a calibration.
- Be aware of total calorie intake as seeing your glucose in real-time can change eating behavior. I found this the case for myself with a CGM in my arm was more likely to avoid that sweet snack or dessert. This may be great if losing weight is ones goal but I found myself losing more weight than I desired during this experiment and this weight loss impacting my hormone levels and overall health in some ways.
- Don't flip out when your glucose rises post meal or hits high levels. I’ll be honest I didn't do great at first with this real-time data on my “health” and had the tendency to be emotionally reactive to my glucose. This gave me anxiety and overall probably worsened my health in retrospect. By the 3rd sensor I was better and was less worried about the data based on my research and acceptance of this.
Summary
I assumed with being extremely active and having very high energy demands I could ignore my metabolic health and diet but after this research and looking at my numbers I do think that this is not fully the case and want to do better at taking care of my metabolic health for the long term. Metabolic health management may be our single best tool for increasing longevity and healthspan as the research linking it to all the most deadly diseases is crystal clear.
This CGM experiment was eye opening and allowed me to better understand how my body reacts to different foods, meal timing, and lifestyle factors like stress and sleep. I felt much more responsible for my food choices when wearing the CGM but this did cause me issues as I subconsciously reduced my caloric intake which led me to undesired weight loss during this experiment. By my 3rd week of using a CGM I was largely used to the readings but early on did have anxiety over watching my glucose levels.
I hope this article will help others with their metabolic health, if they wish to use a CGM or not. I can say that I look at my metabolic health and diet much different after this experiment and that my health and habits are changed for the better.
Thanks for reading and please share with any CGM curious friend and subscribe below to receive an email for future articles like this one.
Other Articles to Check Out:
- Outlive by Peter Attia Key Concepts
- NMN + NR Experiment
- Top Blood Markers For Longevity
- 7 Supplements Actually Backed by Science
Other Sources
https://peterattiamd.com/ama24/
https://www.cell.com/cell-metabolism/pdf/S1550-4131(21)00102-9.pdf https://drguess.substack.com/p/prediabetes-in-athletes
https://peterattiamd.com/cgm-in-non-diabetics/
https://diabetesjournals.org/diabetes/article/57/5/1349/13528/Oscillating-Glucose-Is-More-Deleterious-to
https://www.sciencedirect.com/science/article/pii/S0026049523002445